- Opening hours: 24 Hours
- Call us today: +91 86960-97555
- Email us: info@drsskhatri.com
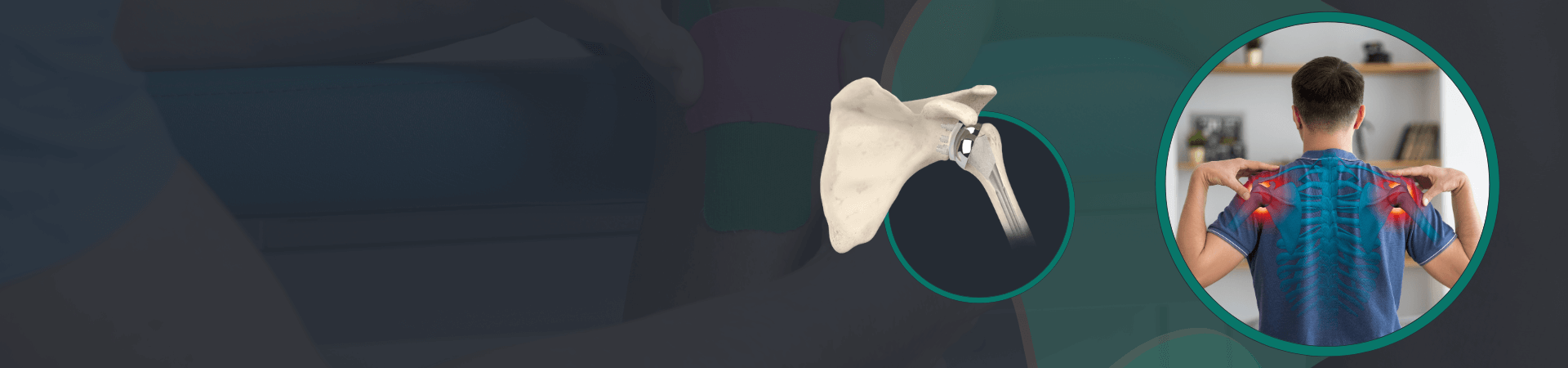
Total shoulder replacement, also known as total shoulder arthroplasty, is a surgical procedure that involves replacing the damaged or diseased shoulder joint with an artificial joint. This procedure is typically recommended for patients who suffer from chronic shoulder pain and stiffness caused by arthritis, rotator cuff tear, or other conditions that damage the shoulder joint.
The procedure is performed under general anesthesia, and the surgeon makes an incision on the front of the shoulder to access the joint. The damaged parts of the shoulder joint, including the ball and socket, are removed and replaced with prosthetic components.
The prosthetic components typically consist of a metal ball attached to a stem that is inserted into the upper arm bone (humerus), and a plastic socket that is fixed into the shoulder blade (scapula). The prosthetic components are designed to mimic the natural shape and movement of the shoulder joint, allowing for improved mobility and pain relief.
After the prosthetic components are implanted, the surgeon will close the incision with sutures or staples, and the patient will be monitored in the recovery room before being transferred to a hospital room or discharged home.
Physical therapy is an essential component of the recovery process after total shoulder replacement. A physical therapist will work with the patient to regain strength, mobility, and range of motion in the shoulder joint. The therapist will also provide guidance on proper shoulder movement and exercise to prevent injury and ensure proper healing.
Overall, total shoulder replacement is a safe and effective procedure for treating chronic shoulder pain and stiffness caused by a variety of conditions. However, as with any surgery, there are risks involved, including infection, bleeding, nerve damage, and joint dislocation. Patients should discuss the potential risks and benefits of the procedure with their surgeon before making a decision to proceed.
Indications:
Total shoulder replacement (also known as shoulder arthroplasty) is recommended for patients with severe shoulder pain and disability caused by degenerative joint disease, rheumatoid arthritis, osteoarthritis, and traumatic injury to the shoulder joint. Other indications include:
- Rotator cuff tear arthropathy
- Avascular necrosis
- Failed previous shoulder surgery
- Severe instability of the shoulder joint
- Fractures of the proximal humerus
- Tumors involving the shoulder joint
Causes:
The most common causes of shoulder joint damage leading to total shoulder replacement are osteoarthritis, rheumatoid arthritis, and post-traumatic arthritis. Osteoarthritis is a degenerative joint disease that affects the cartilage and bones in the shoulder joint, causing pain, stiffness, and loss of motion. Rheumatoid arthritis is a chronic autoimmune disease that causes inflammation and joint damage throughout the body, including the shoulder joint. Traumatic injuries, such as fractures and dislocations, can also cause damage to the shoulder joint, leading to the need for a total shoulder replacement.
Symptoms:
The symptoms of shoulder joint damage that may require a total shoulder replacement include:
- Persistent shoulder pain that limits daily activities and interrupts sleep
- Stiffness and limited range of motion in the shoulder joint
- Weakness and loss of strength in the shoulder muscles
- Grinding, clicking, or popping sounds in the shoulder joint during movement
- Swelling and inflammation around the shoulder joint
- Inability to lift or carry objects with the affected arm.
Overall, proper post-surgical care is crucial for a successful recovery after total shoulder replacement surgery. Follow your doctor’s instructions carefully and report any unusual symptoms or complications promptly.
Get Best & Affordable Treatment.
Get In Touch In The Mean Time.
Our mission is to provide high quality chiropractic care, supportive therapies and nutritional weight loss solutions
Plot No. 7a, Amrapali Marg
Block a,
Vaishali Nagar, Jaipur
Get an Appointment
Team of Professionals




Read Our Latest News & Articles
Find out what’s new and get updates on treatments, procedures, incredible patient stories, and special cases in our blog section.