- Opening hours: 24 Hours
- Call us today: +91 86960-97555
- Email us: info@drsskhatri.com
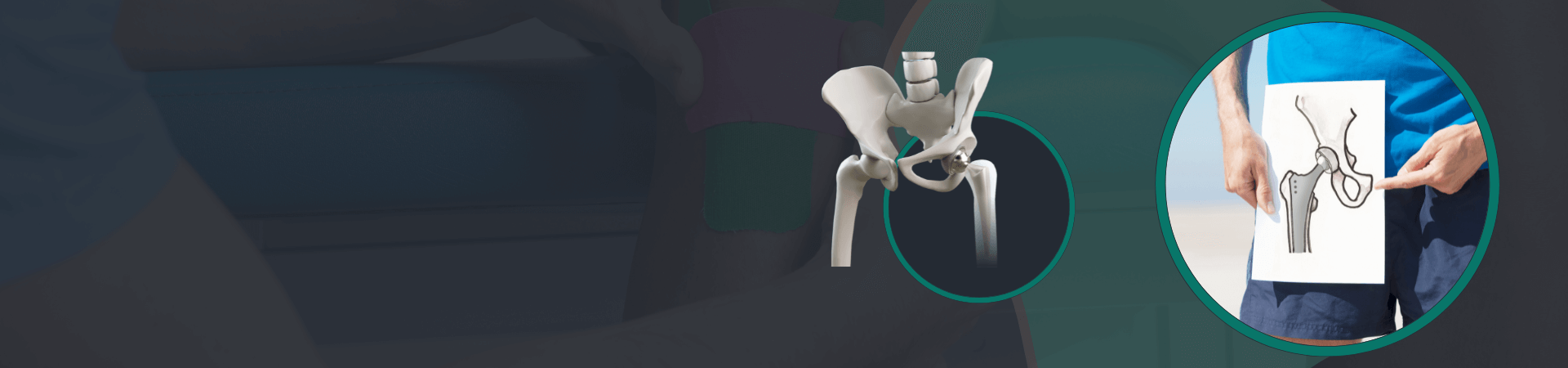
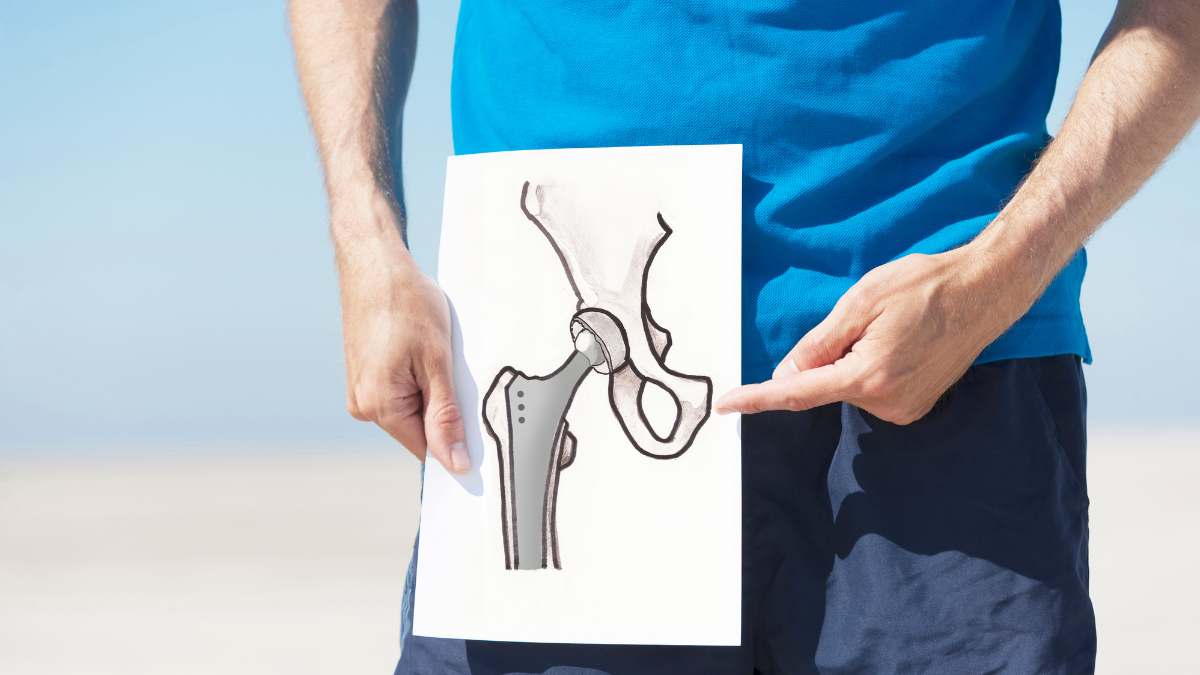
Hip replacement is a surgical procedure in which a damaged or diseased hip joint is replaced with an artificial joint. The hip joint is a ball-and-socket joint, which means that the rounded end of the thighbone (the ball) fits into the cup-shaped socket of the pelvis.
During the surgery, the damaged or diseased ball and socket are removed and replaced with an artificial ball and socket made of metal, plastic, or ceramic. The artificial joint is usually attached to the bone with a special type of cement or is designed to allow the bone to grow into it.
Hip replacement surgery is typically done under general anesthesia, which means you’ll be asleep during the procedure. After the surgery, you’ll likely need to stay in the hospital for a few days and will need physical therapy to help you regain strength and mobility in your hip joint. With proper care and rehabilitation, most people who have hip replacement surgery experience significant improvement in pain, mobility, and quality of life.
When Is A Total Hip Replacement Needed?
A total hip replacement is typically needed when the hip joint has been severely damaged by arthritis, injury, or other conditions that cause pain and limit mobility. Some common reasons why a total hip replacement may be needed include:
- Osteoarthritis: This is the most common reason for hip replacement surgery. Osteoarthritis causes the cartilage that covers the bones in the hip joint to wear down over time, causing pain, stiffness, and difficulty moving.
- Rheumatoid arthritis: This is an autoimmune disorder that causes the body’s immune system to attack the tissues in the joints. Over time, this can cause the cartilage in the hip joint to break down, leading to pain and stiffness.
- Avascular necrosis: This is a condition in which the blood supply to the hip joint is disrupted, causing the bone tissue to die. This can lead to pain, stiffness, and limited mobility.
- Hip fractures: A severe hip fracture can damage the hip joint to the point where a total hip replacement is needed.
- Congenital hip dysplasia: This is a condition in which the hip joint does not develop properly during fetal development. Over time, this can lead to pain, stiffness, and limited mobility.
If you are experiencing persistent hip pain, stiffness, or difficulty moving, you should see a doctor to determine the cause of your symptoms and whether a total hip replacement is needed.
What Are The Potential Risks Associated With Total Hip Replacement?
While total hip replacement is a safe and effective procedure, like any surgical procedure, it carries some potential risks. Some of the potential risks associated with total hip replacement include:
- Infection: Infection is a risk with any surgical procedure. In total hip replacement, the risk of infection is around 1 to 2 percent.
- Blood clots: Blood clots can form in the legs after total hip replacement surgery, which can travel to the lungs and cause a potentially life-threatening condition called pulmonary embolism.
- Dislocation: The new hip joint can become dislocated if the patient makes certain movements or positions that can cause the implant to pop out of the joint.
- Implant failure: The artificial hip joint may wear out over time and fail, requiring revision surgery.
- Nerve damage: During the surgery, there is a risk of nerve damage, which can cause numbness, weakness, or pain.
- Blood loss: Total hip replacement surgery can cause significant blood loss, which can require a blood transfusion.
- Allergic reactions: Some patients may have an allergic reaction to the materials used in the artificial hip joint.
It is important to note that the risk of complications with total hip replacement can be minimized by choosing a skilled surgeon, following post-operative care instructions, and adhering to a rehabilitation plan.
Types of Hip Replacement Surgeries
There are two main types of hip replacement surgeries: unilateral and bilateral.
- Unilateral hip replacement, also known as a partial hip replacement, involves replacing only one hip joint. This is typically done when only one side of the hip joint is damaged or diseased, and the other side is healthy. Unilateral hip replacement surgery usually takes less time and has a shorter recovery period than bilateral hip replacement surgery.
- Bilateral hip replacement, also known as a total hip replacement, involves replacing both hip joints. This is typically done when both sides of the hip joint are damaged or diseased. Bilateral hip replacement surgery is a more extensive procedure and usually requires a longer hospital stay and a longer recovery period than unilateral hip replacement surgery. However, replacing both hip joints at the same time can be beneficial for patients who have difficulty moving around due to pain in both hips.
In summary, unilateral hip replacement involves replacing one hip joint, while bilateral hip replacement involves replacing both hip joints. The choice between the two procedures depends on the patient’s individual condition and needs.
Remember that everyone’s recovery is different, and your doctor may have specific instructions tailored to your individual needs. Be sure to follow all of your doctor’s recommendations for the best possible outcome.
Get Best & Affordable Treatment.
Get In Touch In The Mean Time.
Our mission is to provide high quality chiropractic care, supportive therapies and nutritional weight loss solutions
Plot No. 7a, Amrapali Marg
Block a,
Vaishali Nagar, Jaipur
Get an Appointment
Team of Professionals




Read Our Latest News & Articles
Find out what’s new and get updates on treatments, procedures, incredible patient stories, and special cases in our blog section.